Pulmonary Ventilation Is Best Defined As
Juapaving
Apr 04, 2025 · 6 min read
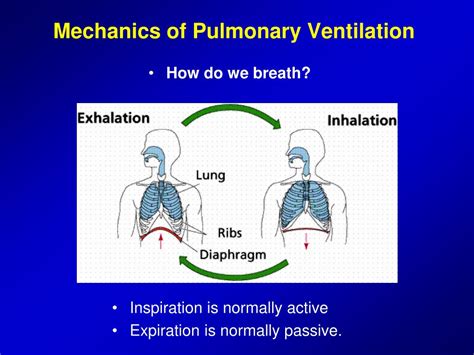
Table of Contents
Pulmonary Ventilation: The Essential Mechanics of Breathing
Pulmonary ventilation, more commonly known as breathing, is the process of moving air into and out of the lungs. It's a seemingly simple act, yet it's a complex interplay of muscular contractions, pressure changes, and sophisticated neurological control that underpins life itself. Understanding pulmonary ventilation is crucial for comprehending respiratory health, disease processes, and the overall functioning of the human body. This article will delve deeply into the mechanics, regulation, and significance of this vital physiological process.
The Mechanics of Pulmonary Ventilation: A Detailed Look
Pulmonary ventilation involves two distinct phases: inspiration (inhalation) and expiration (exhalation). Both are driven by changes in pressure gradients within the thoracic cavity, the space housing the lungs and heart.
Inspiration: Breathing In
Inspiration is an active process, requiring muscular effort to expand the thoracic cavity and reduce the pressure within the lungs. This pressure reduction creates a pressure gradient, drawing air from the atmosphere into the lungs. The key players in inspiration are:
- Diaphragm: This dome-shaped muscle forms the floor of the thoracic cavity. During inspiration, the diaphragm contracts, flattening and moving downwards. This increases the vertical dimension of the thoracic cavity.
- External Intercostal Muscles: Located between the ribs, these muscles contract, lifting the rib cage upwards and outwards. This increases the anteroposterior and lateral dimensions of the thoracic cavity.
- Accessory Muscles: During strenuous breathing or respiratory distress, accessory muscles such as the sternocleidomastoid, scalenes, and pectoralis minor are recruited to assist in further expansion of the chest.
The Pressure Changes: As the thoracic cavity expands, the volume of the lungs increases. According to Boyle's Law, an increase in volume leads to a decrease in pressure. This decreased intrapleural pressure (pressure within the pleural cavity surrounding the lungs) creates a negative pressure relative to atmospheric pressure, drawing air into the lungs until the pressures equalize.
Expiration: Breathing Out
Expiration is generally a passive process at rest. As the inspiratory muscles relax, the elastic recoil of the lungs and chest wall causes the thoracic cavity to decrease in volume. This volume decrease increases the pressure within the lungs, forcing air out into the atmosphere until the pressures equalize.
- Elastic Recoil: The lungs possess inherent elasticity due to the elastic fibers within their tissue and the surface tension of the alveolar fluid. This elastic recoil is a significant driving force of expiration.
- Surface Tension: The thin layer of fluid lining the alveoli (tiny air sacs in the lungs) creates surface tension, which tends to collapse the alveoli. Surfactant, a lipoprotein produced by alveolar cells, reduces surface tension and prevents alveolar collapse.
- Active Expiration: During forceful expiration, such as during exercise or coughing, the internal intercostal muscles and abdominal muscles contract. The internal intercostals pull the ribs downwards and inwards, while the abdominal muscles push the diaphragm upwards, further reducing thoracic cavity volume and increasing pressure for a more forceful exhalation.
Pulmonary Ventilation and Lung Volumes
Understanding lung volumes and capacities is crucial for assessing respiratory function. Several key terms describe the different amounts of air moved during breathing:
- Tidal Volume (TV): The volume of air moved in and out of the lungs during a normal breath.
- Inspiratory Reserve Volume (IRV): The extra volume of air that can be forcefully inhaled after a normal breath.
- Expiratory Reserve Volume (ERV): The extra volume of air that can be forcefully exhaled after a normal breath.
- Residual Volume (RV): The volume of air remaining in the lungs after a forceful exhalation. This air ensures that the alveoli remain partially inflated and prevent complete collapse.
- Inspiratory Capacity (IC): The total volume of air that can be inhaled (TV + IRV).
- Functional Residual Capacity (FRC): The volume of air remaining in the lungs after a normal exhalation (ERV + RV).
- Vital Capacity (VC): The maximum volume of air that can be exhaled after a maximum inhalation (TV + IRV + ERV).
- Total Lung Capacity (TLC): The total volume of air the lungs can hold (TV + IRV + ERV + RV).
These volumes and capacities can be measured using spirometry, a technique used to assess respiratory function and diagnose respiratory diseases.
Regulation of Pulmonary Ventilation
The rate and depth of breathing are precisely controlled to meet the body's metabolic demands. This regulation involves several key components:
Neural Control: The Respiratory Centers
The primary control of breathing resides in the brainstem, specifically in the medulla oblongata and pons. These regions contain clusters of neurons that form the respiratory centers:
- Medullary Respiratory Center: This center generates the basic rhythm of breathing. It contains two groups of neurons: the dorsal respiratory group (DRG) involved in inspiration and the ventral respiratory group (VRG) involved in both inspiration and expiration during forceful breathing.
- Pontine Respiratory Centers: These centers in the pons modulate the output of the medullary centers, smoothing the respiratory rhythm and influencing the transition between inspiration and expiration.
Chemical Control: Sensing Blood Gases
Chemoreceptors, specialized cells sensitive to changes in blood gas levels and pH, play a crucial role in regulating breathing:
- Central Chemoreceptors: Located in the medulla, these receptors are sensitive to changes in carbon dioxide (CO2) levels and pH in the cerebrospinal fluid. Increased CO2 leads to increased acidity (lower pH), stimulating these receptors and increasing the rate and depth of breathing.
- Peripheral Chemoreceptors: Located in the carotid and aortic bodies, these receptors are sensitive to changes in both CO2 and oxygen (O2) levels, as well as pH in arterial blood. Decreased O2 levels or increased acidity stimulate these receptors, leading to increased ventilation.
Other Influences on Ventilation
Several other factors can influence breathing rate and depth, including:
- Stretch Receptors: Located in the lungs, these receptors detect lung inflation and trigger a protective mechanism called the Hering-Breuer reflex, preventing overinflation of the lungs.
- Irritant Receptors: Located in the airways, these receptors are sensitive to irritants such as dust, smoke, and noxious gases. Stimulation of these receptors leads to coughing, bronchoconstriction, and increased ventilation.
- Higher Brain Centers: The cerebral cortex can exert voluntary control over breathing, allowing conscious control of breathing patterns. However, this voluntary control is limited and cannot override the basic respiratory rhythm generated by the brainstem.
- Emotional Factors: Stress, anxiety, and pain can alter breathing patterns, often leading to increased ventilation.
Clinical Significance of Pulmonary Ventilation Disorders
Impaired pulmonary ventilation can have serious consequences. Various conditions can affect the ability to adequately move air in and out of the lungs, leading to:
- Hypoventilation: Reduced alveolar ventilation, leading to increased CO2 and decreased O2 levels in the blood. This can lead to respiratory acidosis, hypoxia, and potentially death.
- Hyperventilation: Increased alveolar ventilation, leading to decreased CO2 and increased O2 levels in the blood. This can lead to respiratory alkalosis, dizziness, and even seizures.
- Asthma: Chronic inflammatory disease of the airways causing bronchoconstriction and airway inflammation, leading to reduced airflow and difficulty breathing.
- Chronic Obstructive Pulmonary Disease (COPD): Group of diseases characterized by persistent airflow limitation, including chronic bronchitis and emphysema.
- Pneumonia: Infection of the lungs, causing inflammation and fluid buildup in the alveoli, impairing gas exchange.
- Pleurisy: Inflammation of the pleural membranes surrounding the lungs, causing pain and impaired breathing.
- Pneumothorax: Collapse of a lung due to air leaking into the pleural cavity.
Conclusion: The Vital Role of Pulmonary Ventilation
Pulmonary ventilation is a fundamental physiological process essential for life. Its intricate mechanics, precise regulation, and susceptibility to various disorders highlight its importance in maintaining overall health. Understanding the complexities of breathing is paramount for appreciating the delicate balance necessary for respiratory health and the critical role it plays in the body's overall function. Further research and advancements in understanding pulmonary ventilation will continue to improve diagnosis, treatment, and prevention of respiratory diseases.
Latest Posts
Latest Posts
-
Which Graph Has A Slope Of 4 5
Apr 04, 2025
-
11 Cm Is How Many Inches
Apr 04, 2025
-
How Tall Is 30 Inches In Feet
Apr 04, 2025
-
The Speed Of Light In A Vacuum Is
Apr 04, 2025
-
What Is The Largest Animal On Land
Apr 04, 2025
Related Post
Thank you for visiting our website which covers about Pulmonary Ventilation Is Best Defined As . We hope the information provided has been useful to you. Feel free to contact us if you have any questions or need further assistance. See you next time and don't miss to bookmark.
