This Is The Functional Unit Of The Kidney
Juapaving
Apr 03, 2025 · 8 min read
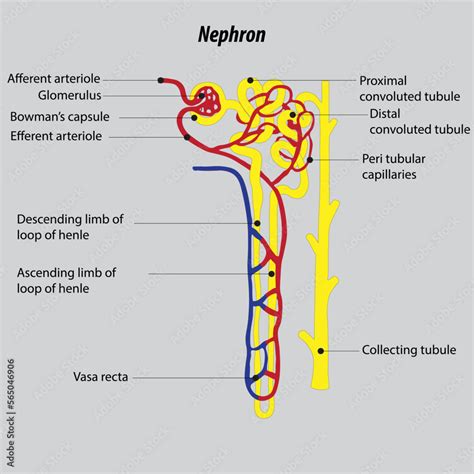
Table of Contents
The Nephron: The Functional Unit of the Kidney
The kidney, a vital organ in the human body, plays a crucial role in maintaining homeostasis. It achieves this remarkable feat through a complex network of processes, all centered around its fundamental functional unit: the nephron. Understanding the nephron is key to comprehending how the kidneys filter blood, regulate blood pressure, maintain electrolyte balance, and eliminate waste products. This article delves deep into the structure, function, and processes within the nephron, exploring its intricate mechanisms and their significance in overall health.
Anatomy of the Nephron: A Detailed Look
Each kidney houses approximately one million nephrons, and their combined action determines the kidney's overall function. These microscopic units are responsible for the intricate process of urine formation. A nephron consists of two main parts:
1. Renal Corpuscle: The Filtration Site
The renal corpuscle, also known as the Bowman's capsule, marks the beginning of the nephron. It comprises:
-
Glomerulus: A network of capillaries where blood filtration begins. The glomerulus's specialized structure, featuring fenestrated capillaries (with pores), allows for efficient passage of water and small solutes while effectively retaining larger molecules like proteins and blood cells. The high pressure within the glomerulus facilitates this crucial filtration process. The afferent arteriole, larger in diameter than the efferent arteriole, contributes significantly to this pressure differential.
-
Bowman's Capsule: A double-walled cup-like structure surrounding the glomerulus. The visceral layer of the Bowman's capsule, composed of specialized cells called podocytes, plays a crucial role in regulating filtration. Podocytes possess foot-like processes that interdigitate, creating filtration slits that further refine the filtering process. The parietal layer forms the outer wall of the Bowman's capsule. The space between these layers is known as the Bowman's space, where the filtered fluid (glomerular filtrate) collects.
2. Renal Tubule: Reabsorption and Secretion
After passing through the Bowman's capsule, the filtrate enters the renal tubule, a long, convoluted structure divided into distinct segments:
-
Proximal Convoluted Tubule (PCT): The PCT is characterized by its extensive microvilli, increasing its surface area for reabsorption. The majority of reabsorption occurs here, including essential nutrients like glucose, amino acids, and ions (sodium, potassium, chloride, bicarbonate). Water is also reabsorbed passively, following the movement of solutes. The PCT also actively secretes certain substances, such as hydrogen ions and drugs.
-
Loop of Henle: This U-shaped structure extends into the renal medulla, creating a concentration gradient crucial for concentrating urine. The descending limb is highly permeable to water but less permeable to solutes, while the ascending limb is impermeable to water but actively transports sodium, potassium, and chloride ions out of the filtrate. This countercurrent mechanism establishes the medullary osmotic gradient, a key feature in regulating urine concentration.
-
Distal Convoluted Tubule (DCT): The DCT is responsible for fine-tuning electrolyte balance and pH regulation. It actively reabsorbs sodium and calcium ions and secretes potassium and hydrogen ions. The DCT is also highly sensitive to hormones such as aldosterone and parathyroid hormone, which influence its reabsorption and secretion activities.
-
Collecting Duct: The collecting duct receives filtrate from multiple nephrons. It plays a crucial role in regulating water reabsorption and ultimately determining the final concentration of urine. The permeability of the collecting duct to water is regulated by antidiuretic hormone (ADH), also known as vasopressin. ADH increases water reabsorption, producing concentrated urine; its absence leads to dilute urine.
Processes within the Nephron: Filtration, Reabsorption, Secretion
The nephron performs three key processes to maintain homeostasis:
1. Glomerular Filtration: The Initial Step
Glomerular filtration is the first step in urine formation. The high pressure within the glomerulus forces water and small solutes from the blood into Bowman's space, forming the glomerular filtrate. This filtrate initially resembles blood plasma but lacks large proteins and blood cells. The glomerular filtration rate (GFR) is a crucial indicator of kidney function.
2. Tubular Reabsorption: Reclaiming Essential Substances
Tubular reabsorption is the process of selectively retrieving essential substances from the glomerular filtrate back into the bloodstream. This crucial process occurs along the renal tubule and involves both passive and active transport mechanisms. Nutrients, water, and electrolytes are reabsorbed, ensuring their retention in the body. The specific transport mechanisms vary along the different segments of the renal tubule.
3. Tubular Secretion: Eliminating Unwanted Substances
Tubular secretion is the active transport of specific substances from the peritubular capillaries (the capillaries surrounding the renal tubules) into the renal tubule. This process is essential for eliminating waste products, toxins, and excess ions that were not initially filtered or that need to be removed from the bloodstream. Hydrogen ions, potassium ions, and certain drugs are actively secreted into the tubule.
Hormonal Regulation of Nephron Function: Maintaining Balance
Several hormones play critical roles in regulating nephron function and maintaining fluid and electrolyte balance:
-
Antidiuretic Hormone (ADH): ADH, released by the posterior pituitary gland, increases the permeability of the collecting duct to water, promoting water reabsorption and producing concentrated urine. This is crucial in maintaining fluid balance during dehydration.
-
Aldosterone: Aldosterone, a mineralocorticoid hormone secreted by the adrenal cortex, increases sodium reabsorption in the distal convoluted tubule and collecting duct. This leads to increased water retention and blood pressure regulation.
-
Parathyroid Hormone (PTH): PTH, secreted by the parathyroid glands, increases calcium reabsorption in the distal convoluted tubule. This is vital for maintaining calcium homeostasis.
-
Atrial Natriuretic Peptide (ANP): ANP, secreted by the heart atria in response to high blood volume, inhibits sodium reabsorption in the collecting duct, leading to increased sodium and water excretion, reducing blood pressure.
Clinical Significance: Understanding Kidney Diseases
Nephron dysfunction can lead to various kidney diseases, including:
-
Glomerulonephritis: Inflammation of the glomeruli, causing damage to the filtration membrane and leading to proteinuria (protein in urine) and hematuria (blood in urine).
-
Acute Kidney Injury (AKI): Sudden loss of kidney function, often caused by dehydration, infection, or medications.
-
Chronic Kidney Disease (CKD): Progressive loss of kidney function over time, often due to diabetes, hypertension, or other underlying conditions. CKD can lead to end-stage renal disease (ESRD), requiring dialysis or kidney transplantation.
Understanding the structure and function of the nephron is critical for diagnosing and managing kidney diseases. Early detection and management are crucial to slowing disease progression and improving patient outcomes.
The Juxtaglomerular Apparatus: Local Regulation
The juxtaglomerular apparatus (JGA) is a specialized structure located where the distal convoluted tubule comes into contact with the afferent and efferent arterioles of the same nephron. This apparatus plays a critical role in the autoregulation of glomerular filtration rate (GFR) and blood pressure.
The JGA is composed of three key cell types:
-
Juxtaglomerular cells: Modified smooth muscle cells located in the walls of the afferent arteriole. These cells secrete renin, an enzyme that plays a key role in the renin-angiotensin-aldosterone system (RAAS). Renin initiates a cascade that ultimately leads to increased blood pressure and sodium reabsorption.
-
Macula densa: Specialized epithelial cells located in the distal convoluted tubule. These cells monitor the sodium chloride concentration in the filtrate. Changes in sodium chloride concentration trigger the release of renin from the juxtaglomerular cells.
-
Extraglomerular mesangial cells: These cells connect the macula densa and juxtaglomerular cells. They are thought to play a role in communication between these two cell types.
The JGA's role in maintaining GFR and blood pressure is crucial. When blood pressure drops, the JGA releases renin, leading to increased blood pressure. Conversely, when blood pressure is too high, the JGA reduces renin secretion. This intricate feedback mechanism helps maintain blood pressure within a normal range.
Variations in Nephron Structure: Cortical vs. Juxtamedullary Nephrons
Nephrons are not all created equal. Two main types of nephrons exist:
-
Cortical Nephrons: These are the most abundant type of nephron, located primarily in the renal cortex. They have short loops of Henle that extend only slightly into the medulla. They are primarily involved in the filtration and reabsorption of fluids and electrolytes.
-
Juxtamedullary Nephrons: These nephrons have long loops of Henle that extend deep into the renal medulla. Their long loops of Henle are essential for establishing the concentration gradient in the medulla, which is crucial for concentrating urine. This ability to concentrate urine is critical for conserving water.
The difference in loop length directly influences the kidney's ability to concentrate urine. Juxtamedullary nephrons are particularly important in maintaining water balance during periods of dehydration.
Conclusion: The Nephron's Essential Role in Kidney Function
The nephron is the fundamental functional unit of the kidney, performing a multitude of complex tasks to maintain homeostasis. Its intricate structure and the coordinated actions of its various segments ensure the efficient filtration of blood, the reabsorption of essential substances, and the secretion of waste products. Understanding the nephron's structure and function is paramount for comprehending kidney physiology and the pathogenesis of kidney diseases. Further research into the intricacies of nephron function continues to reveal new insights into the remarkable processes that maintain our health. The nephron's remarkable capacity to adapt and respond to changes in the body's internal environment underscores its vital role in overall well-being. Maintaining healthy kidney function through a healthy lifestyle is crucial for preserving overall health and preventing kidney-related diseases.
Latest Posts
Latest Posts
-
What Lays Eggs And Is Not A Bird
Apr 04, 2025
-
An Alternate Form Of A Gene
Apr 04, 2025
-
How Many Joules In A Kilowatt Hour
Apr 04, 2025
-
1 Nucleic Acids Are Polymers Of
Apr 04, 2025
-
How Many Centimeters Are In 2 M
Apr 04, 2025
Related Post
Thank you for visiting our website which covers about This Is The Functional Unit Of The Kidney . We hope the information provided has been useful to you. Feel free to contact us if you have any questions or need further assistance. See you next time and don't miss to bookmark.
